Perspective Fallacy COVID
Every now and then hear speculations about the changing nature of COVID19. Clinicians say that they are getting more and more younger patients, but official studies do not support the claim that the Delta variant shifted the odds in any direction. Clinicians say that they have information faster, scientists say only robust large sample historical data can give us full picture. Let's look at data right before the vaccination program started and right after there were at least 50% of fully vaccinated population. This should give us information on whether there were actually any shifts in trends.
The Method
Data from CDC was used Case Surveillance Public Use Data. The vaccination program in US was launched mid December 2020 and reached 50% fully vaccinated people in August 2021. So 3 months prior to the start - October, November and December 2020 - were compared against 3 months right after this symbolic goal was reached - August, September and October 2021.
The analysis rests on a naive assumption that the testing strategy remained largely unchanged. It also does not take into account different vaccination rates in different age groups.
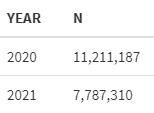
In these two periods the numbers of cases differed. The sample from 2020 is larger than that from 2021 - 11,211,187 vs 7,787,310.
I don't recommend focusing on exact numbers due to medium-low quality of the data. The purpose of this analysis is to show how much our conclusions are affected by our perspective and why it is important to strive for a wider perspective in analyzing trends.
Hospitalizations
First, let’s look from a clinician’s perspective. How, if at all, did the proportion of different age groups change over time?
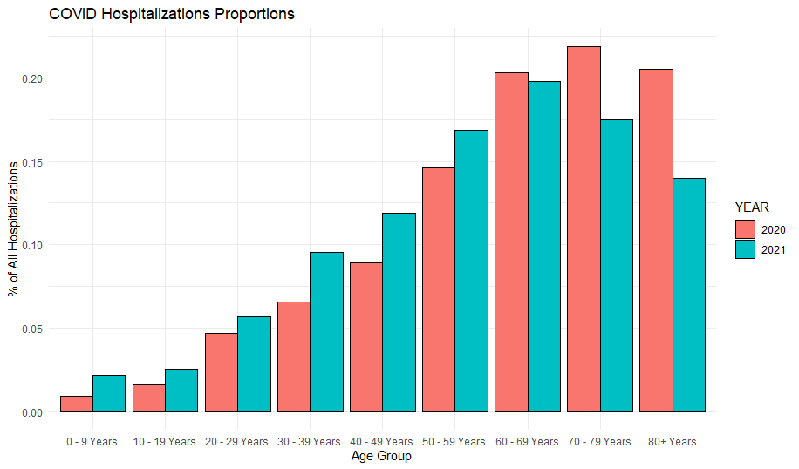
The three highest age groups all contributed more than 20% of all hospitalization alone. It means that together the combined age group of 60+ constituted well over 60% of all hospitalizations. We can see that in 60+ age groups the relative number of hospitalizations decreased, especially for the highest age group, but increased in 0-60 groups. So from a clinician’s perspective it is right that COVID harms more and more younger people.
However, you can easily argue that a doctor doesn’t see all the patients that don’t need to be in a hospital so he doesn’t really know how many people get infected and how many of them are admitted to the hospital. Let’s calculate the risk of hospitalization per age group to see if the risk of hospitalization has changes over time.
Hospitalization risk = number of hospitalization / number of infections
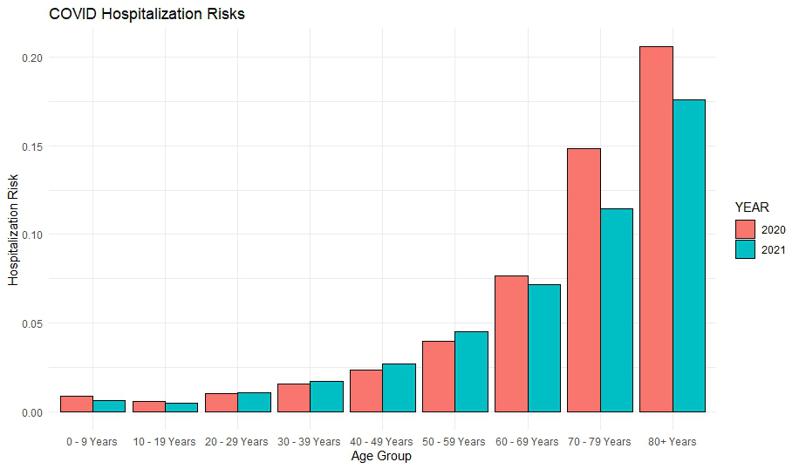
We can see that this approach paints a very different picture. The case / hospitalization ratio notably decreased for the two highest age groups but all other differences are negligible. The two lowest age groups, while increased their proportion in hospitalizations, have even slightly lower risk of hospital admission than before. We can assume that this is just natural fluctuation in the data as the lowest age group was not even eligible for inoculation, so vaccination didn’t impact the result.
ICU (Intesive Care Unit) Admissions
Hospitalizations admission criteria can be flexible. If there is an abundance of beds, the criteria are lax. When there is shortage, all that can be sent home are sent home. The criteria for ICU are more rigid and less prone to the discretion of the doctor.
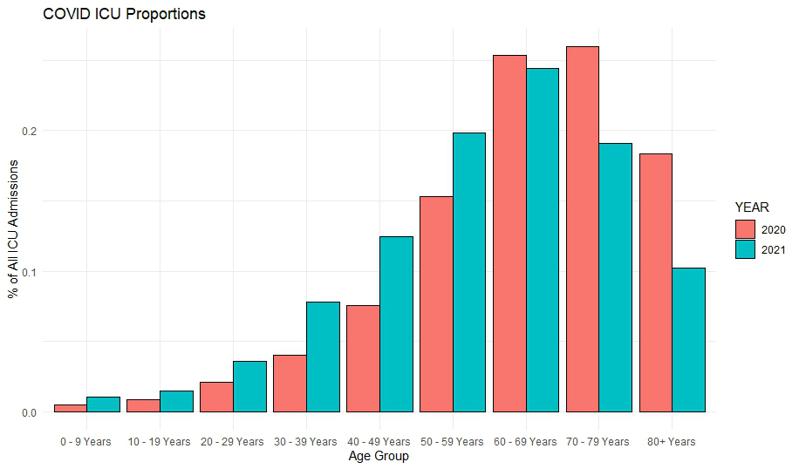
Like in the case of hospitalization, highest age groups are less frequent today than last year. It seems the younger people are now more frequently admitted then before. Surprisingly, the 60-69 and 70-79 age group dominate the ICU and not the 80+ group.
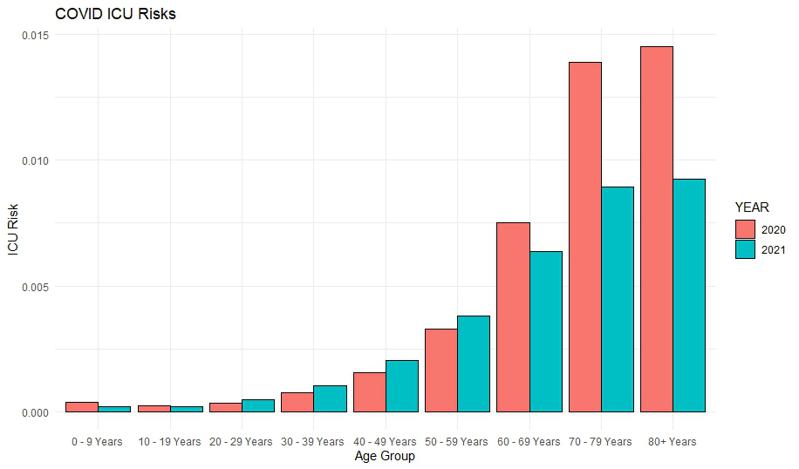
Similarly as in case of hospitalization, the risk analysis using full data does not support the claim that there is visible increase in risk for lower age groups. However, the risk of being admitted to ICU for the two highest risk groups was reduced by a third.
Deaths
The last category is the most captivating - number of deaths.
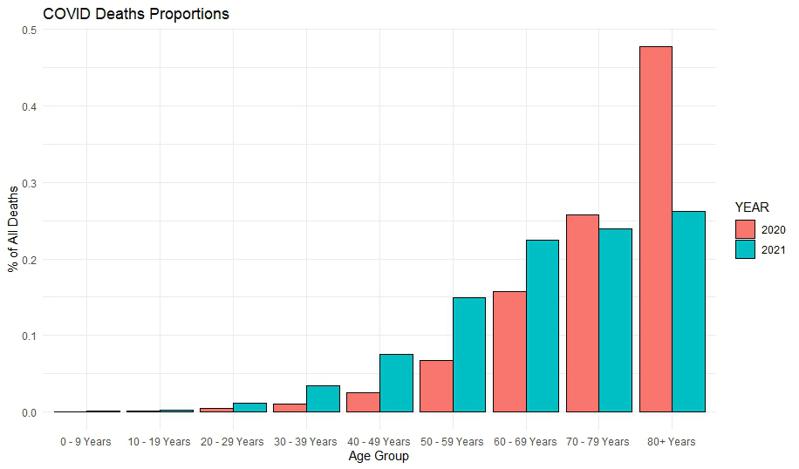
This above chart should not surprise anyone who follows the COVID deaths statistics. The median age of a deceased COVID patient is not much below the expected lifetime. Nearly half of all the deaths prior to the vaccination program were among the 80+ years of age. That proportion has been reduced by half. But does that mean half the risk?
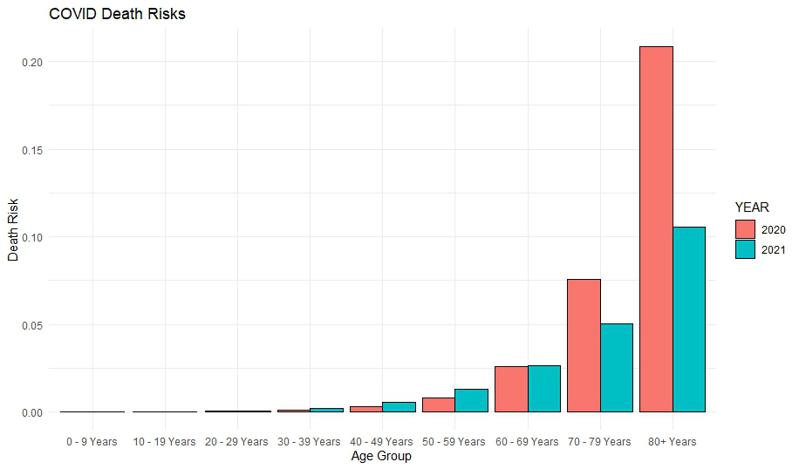
It seems that indeed, it does mean half the risk for 80+ years of age. From initial ~20% case / fatality ratio, which is consistent with early estimates from Fatality rate of novel coronavirus COVID-19 in China as of February 11, 2020, by age group, to half that - around 10%. There is also a reduction in risk by a third in the 70-79 group. Surprisingly, these are the only age groups actually benefiting in terms of reduced risk of death. There seems to be no difference so far in other relatively high-risk age groups - 50+.
PS
You might still argue that this is because of low vaccination rates among certain age groups. You can argue that now mainly unvaccinated people get infected and subsequently are admitted to the hospital. We have no data on how many vaccinated and unvaccinated people get infected and how severe their infections are. But if we look at the data it actually shows that the highest age groups have very high level of vaccination rates.
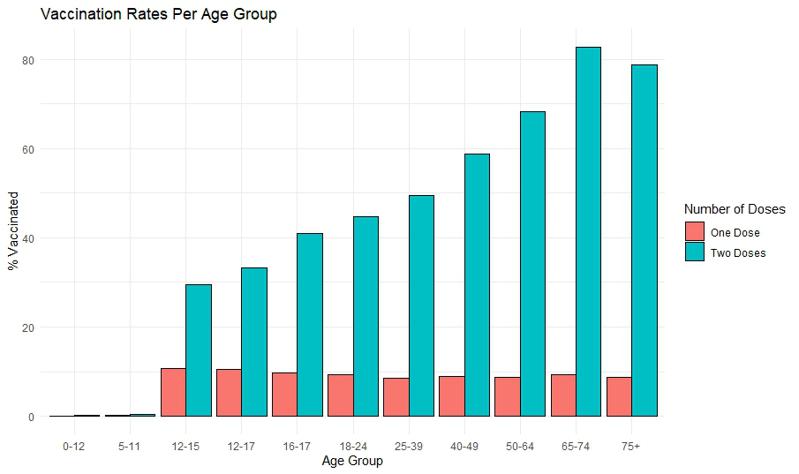
Data as of 2021-08-01 from CDC
People above 50 years of age generally have a vaccination rate above 75%. The 80+ years group benefited greatly from the vaccinations in terms of risk reduction. However, this does not seem to be true for other age groups that have even higher vaccination rates, such as 65-74.
Conclusions
The first conclusion is that a small slice of reality, i.e. from a single hospital’s perspective, does not necessarily reflect the broader reality. This is actually why Evidence Based Medicine was devised in the first place. Only samples of sufficient size and drawn from wider population can give us a full picture. While it may look from a doctor’s perspective that COVID patients are getting younger, it is because he doesn’t take into consideration the fact that higher age groups were vaccinated first and that the risk reduction in those groups was the highest, therefore shifting the balance of age.
The second conclusion is that so far only the very highest age groups benefited from the vaccinations. Nearly 50% of deaths before the vaccine occurred among the 80+ group. Today that number is half that. It seems that most of the drop in case / fatality ratio is due to the risk reduction only in the highest age groups. Surprisingly, all other age groups have not really benefited from vaccines in terms of death risk reduction. But that conclusion requires more in-depth analysis.
